An ingrown toenail can become infected if the nail causes a break in the skin. The opening in the skin allows bacteria to enter the tissues under the skin. These bacteria will multiply and destroy the tissues which cause the body to react with inflammation. This is the main mechanism of ingrown toenail infection.
Human skin is a barrier for microorganisms. Some bacteria can be normally found on human skin. The most dominant one is Staphylococcus epidermis. Other types of bacteria that can be found on human skin are micrococci, Pseudomonas, diphtheroid. They will not cause any symptoms if they stay only on the skin. If the skin is intact, it will prevent bacteria and other microorganisms to enter the human body.
Stages of Ingrown Toenail Infection
In the first stage of an infected ingrown nail, the microorganism which entered the toe will start multiplying and destroying the surrounding tissue. It will cause the migration of the inflammatory cells from the blood to the site of infection. In this stage, the human immune system will battle the microorganism to prevent further development of infection. That will lead to swelling, redness and tenderness of the toe.
If the patient is immune-compromised, if the infection is not treated properly, if the microorganism is resistant to treatment methods or if the microorganism is multiplying faster than it is being destroyed then the infection will last for a longer period of time. This will cause the accumulation of the human immune cells from the blood and bacteria from the skin. As the battle between them lasts longer it leads to an accumulation of dead matter in the toe. The dead matter are destroyed bacteria, immune cells, and tissue which was destroyed by bacteria. They form a clear/yellow liquid called pus which will start draining from the infected ingrown toenail.
If the infection continues then granulation tissue will be formed. The formation of granulation tissue will start after the special cells from the human blood, called fibroblasts, migrate to the site of infection. There are also other immune cells in granulation tissue. As the granulation tissue grows it covers the site of pus drainage and in that way it prevents drainage. This will eventually lead to recurrence of infection.
The infected ingrown toenail will be swollen, red and extremely painful to touch or pressure. In the second stage, at the site of ingrowing toenail, pus will start draining. In the beginning, it will be firmer and in later stages, it will probably be yellowish or greenish, sticky and it will smell unpleasant. If the infection progresses to stage three, at the site of infection a new tissue will form. It will be pinkish colored and may bleed.
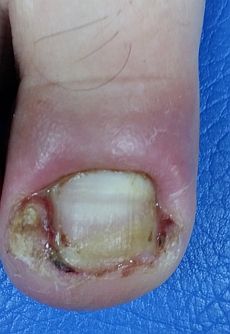
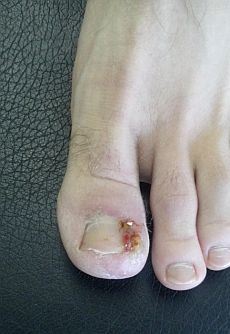
Samples of infected ingrown toenails
Infections Caused by an Ingrown Toenail
Paronychia
Depending on the spread of microorganisms in the human body there are several forms of infection which can be caused by an ingrown toenail. Local infection of the soft tissue of the side of the toe is called paronychia. The mechanism of paronychia infection caused by the ingrown toenail is described above in the text. Shortly, microorganisms enter the soft tissue on the side of the toe through a wound which was created by an ingrown toenail. There they will multiply and fight with the immune cells which will lead to infection and pus formation. There are also other causes of paronychia: nail biting, sucking thumbs by infants and manicures/pedicures.
In the acute form of paronychia, ingrown toenail infection will spread in a few hours and it will lead to abscess formation. If the infected ingrown toenail is more severe it can cause fever and enlargement of lymph nodes. The most common causes are Staphylococcus. In the chronic form, the process will go more slowly. It will eventually lead to inflammation of the toe and may eventually lead to the destruction of the nail plate. In this case, fungal infection is more common.
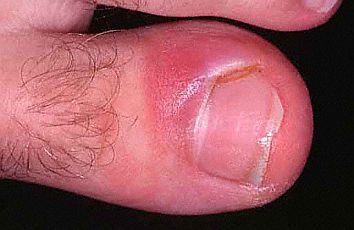
Paronychia, Hardin Library for the Health Sciences, 2010, available from http://hardinmd.lib.uiowa.edu/dermnet/paronychia2.html
Cellulitis
Cellulitis is an infection of the skin. It can be caused by bacteria which entered the body after the toenail was ingrown. Cellulitis will be located on the side of the ingrown nail. The whole foot can be swollen, red, painful and warm. If it is untreated it can be very dangerous and it may lead to bacteremia and sepsis (bacteria spread through the entire body which can lead to organ failure). The diagnosis can be made by physical assessment. Antibiotic treatment should be started immediately.
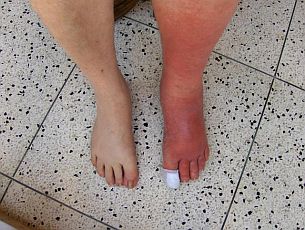
Cellulitis, available from http://www.redefiningthefaceofbeauty.com/2013/05/skin-disorders-cellulitis.html
Diagnosis of Ingrown Toenail Infection
If you have any symptoms of ingrown toenail infection you should visit your physician. This condition can be diagnosed by local inspection of the toe. If the ingrown toenail is already in the abscess stage then a wound swab should be taken to confirm the diagnosis and to find which microorganism causes it. This will also help the physician to prescribe the appropriate antibiotic which will treat the infected ingrown toenail.
Treatment of Ingrown Toenail Infection
There are several methods for treatment of an infected ingrown toenail. If the toe is still not too infected then one of the first methods which should be used is soaking of the toe. The foot can be soaked in warm water for ten minutes and repeated several times per day. It will soften the skin on the side of the toe in where the toenail is ingrown. That will allow the patient to retract the skin and expose the side of the toenail. You can also add Epsom salt or antibacterial solutions into the water. This method can be helpful for treatment of the first stage of an ingrown toenail. Cotton can be used to elevate the ingrown part of the nail.
If there are signs of infection then local antibiotic therapy can be started. This can be helpful in some milder cases of infection. The most commonly used topical antibiotic is Neosporin.
In the case of more severe infection, oral antibiotic therapy is indicated. Oral broad spectrum antibiotics should be prescribed to try to reduce the infection. Swab culture can be helpful in determining which antibiotic should be prescribed.
In case any of the conservative measures do not show progress in the treatment of ingrown toenail infection then surgery is the only solution. There are a variety of different surgical techniques which can be used to treat an infected ingrown toenail.
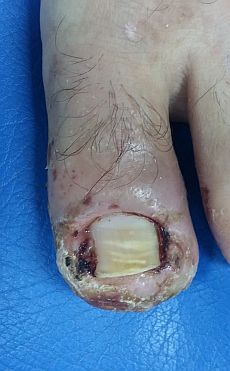
Infected ingrown toenail after unsuccessful oral and topical antibiotic therapy
Preventing Infection of an Ingrown Toenail
The best prevention of ingrown toenail infection is preventing the occurrence of the ingrown toenail in the first place. Practice proper foot care. Wear shoes and socks that do not fit tightly. Toenails should be trimmed straight across. Ingrown toenails should be treated before ingrown toenail infection is allowed to occur. It should be soaked and washed more frequently. The foot should always be dry. At the first sign if an infected ingrown toenail, you should visit your physician.
References:
American Orthopedic Foot and Ankle Society: Ingrown Toenail, 2012, available online at http://orthoinfo.aaos.org/topic.cfm?topic=a00154
Blahd H, Ingrown toenail – Topic overview, March 12, 2014, available online at http://www.webmd.com/skin-problems-and-treatments/tc/ingrown-toenail-topic-overview?page=1
Davis CP: Normal flora, Chapter 6 in Medical Microbiology. 4th edition, 1996, Galveston (TX)
Gary W. Cole GW: Ingrown Toenails, 2016, available online at http://www.emedicinehealth.com/ingrown_toenails/page9_em.htm
Healthunlocked: Abscess – Causes, reviewed 2014, available online at http://www.nhs.uk/Conditions/Abscess/Pages/Causes.aspx
Hon A, Paronychia, Updated September 2015, available online at http://www.dermnetnz.org/fungal/paronychia.html
NHS Choices: Ingrown toenail, 2014, available online at http://www.nhs.uk/conditions/Ingrown-toenail/Pages/Introduction.aspx
Radovic PA: Ingrown Toenail (Onychocryptosis), 2015, available online at http://www.medicinenet.com/ingrown_toenail/page9.htm
Stanway A, Cellulitis , June 2014., available online at http://www.dermnetnz.org/bacterial/cellulitis.html
